Return to flip book view
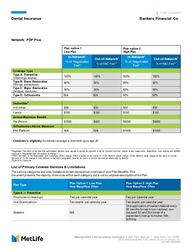
Metropolitan Life Insurance Company | 200 Park Avenue | New York, NY 10166 L0521014040[exp0622][xNM ] © 2021 MetLife Services and Solutions, LLC DN-ANY-PPO-DU AL PLAN SUMMARY Dental Insurance Bankers Financial Co. Network: PDP Plus Deductible† Individual $50 $50 $50 $50 Family $150 $150 $150 $150 Annual Maximum Benefit Per Perso n $1000 $500 $5000 $5000 Orthodontia Lifetime Maximum Per Person N/A N/A $1500 $1500 Child(ren)’s eligibility for dental coverage is from birth up to age 26 *Neg otiated Fee refers to the fees that participating dentists have ag reed to accept as payment in full for covered services, subject to any copayments, deductibles, cost sharing and benefits maximums. Neg otiated fees ar e subject to chang e. ***R&C fee r efers to the Reasonable and Customary (R&C) charge, which is based on the lowest of ( 1) the dentist’s actual char ge, (2) the dentist’s usual charg e for the sam e or similar services, or (3) the charg e of most dentists in the sam e g eog raphic area for the sam e or sim ilar services as determined by M etLife. †Type B & C Services. List of Primary Covered Services & Limitations The service categories and plan limitations shown represent an overview of your Plan Benefits. This document presents the majority of services within each category, but is not a complete description of the Plan. Plan option 1 Low Plan Plan option 2 High Plan In-Network1 % of Negotiated Fee2 Out-of-Network1 % of R&C Fee** In-Network1 % of Negotiated Fee2 Out-of-Network1 % of R&C Fee** Coverage Type Type A: Preventive (cleanings, exams) 100% 100% 100% 100% Type B: Basic Restorative (fillings, extractions) 80% 50% 90% 60% Type C: Major Restorative (bridges, dentures) 50% 25% 60% 50% Type D: Orthodontia N/A N/A 50% 50% Plan Type Plan Option 1: Low Plan How Many/How Often Plan Option 2: High Plan How Many/How Often Type A — Preventive Prophylaxis (cleanings) Two per calendar year Two per calendar year Oral Examinations Two exams per calendar year Two exams per calendar year Sealants N/A One application of sealant material every 60 months for each non-restored, non-decayed 1st and 2nd molar of a dependent child up to his/her 16th birthday
Metropolitan Life Insurance Company | 200 Park Avenue | New York, NY 10166 L0521014040[exp0622][xNM ] © 2021 MetLife Services and Solutions, LLC DN-ANY-PPO-DU AL PLAN SUMMARY Dental Insurance Bankers Financial Co. Topical Fluoride App lications One fluoride treatment per calendar year for dependent children up to his/her 16th birthday One fluoride treatment per calendar year for dependent children up to his/her 16th birthday X-rays N/A Full mouth X-rays; one per 5 calendar years Bitewings X-rays; one set per calendar year Space Maintainers Space maintainers for dependent children up to his/her 16th birthday once per tooth area per lifetime Space maintainers for dependent children up to his/her 16th birthday once per tooth area per lifetime Type B — Basic Restorative Fillings Once every 24 months Once every 24 months Periodontics N/A Periodontal scaling and root planing once per quadrant, every 24 months Periodontal surgery once per quadrant, every 36 months Total number of periodontal maintenance treatments and prophylaxis cannot exceed four treatments in a calendar year X-rays Full mouth X-rays; one per 5 calendar years Bitewings X-rays; one set per calendar year Simple Extractions Crown, Denture and Bridge Repair/ Recementations Endodontics Once per tooth per lifetime Once per tooth per lifetime Oral Surgery N/A Sealants One application of sealant material every 60 months for each non-restored, non-decayed 1st and 2nd molar of a dependent child up to his/her 16th birthday N/A Type C — Major Restorative Oral Surgery N/A Implants Replacement once every 5 years Replacement once every 5 years Bridges and Dentures Initial placement to replace one or more natural teeth, which are lost while covered by the plan Dentures and bridgework replacement; one every 5 calendar years Replacement of an existing temporary full denture if the temporary denture cannot be repaired and the permanent denture is installed within 12 months after the temporary denture was installed Initial placement to replace one or more natural teeth, which are lost while covered by the plan Dentures and bridgework replacement; one every 5 calendar years Replacement of an existing temporary full denture if the temporary denture cannot be repaired and the permanent denture is installed within 12 months after the temporary denture was installed Crowns, Inlays and Onlays Replacement once every 5 calendar years Replacement once every 5 calendar years
Metropolitan Life Insurance Company | 200 Park Avenue | New York, NY 10166 L0521014040[exp0622][xNM ] © 2021 MetLife Services and Solutions, LLC DN-ANY-PPO-DU AL PLAN SUMMARY Dental Insurance Bankers Financial Co. Endodontics N/A General Anesthesia When dentally necessary in connection with oral surgery, extractions or other covered dental services When dentally necessary in connection with oral surgery, extractions or other covered dental services Periodontics Periodontal scaling and root planing once per quadrant, every 24 months Periodontal surgery once per quadrant, every 36 months Total number of periodontal maintenance treatments and prophylaxis cannot exceed four treatments in a calendar year N/A
Metropolitan Life Insurance Company | 200 Park Avenue | New York, NY 10166 L0521014040[exp0622][xNM ] © 2021 MetLife Services and Solutions, LLC DN-ANY-PPO-DU AL PLAN SUMMARY Dental Insurance Bankers Financial Co. The service categ or ies and plan limitations shown above represent an overview of your plan benefits. This document presents the m ajority of services within each categ ory, but is not a com plete description of the plan. ExclusionsThis plan does not cover the following services, treatments and supplies: • Services which are not Dentally Necessary, those which do not meet generally accepted standards of care for treating the particular dental condition, or which we deem experimental in nature; • Services for which you would not be required to pay in the absence of Dental Insurance; • Services or supplies received by you or your Dependent before the Dental Insurance starts for that person; • Services which are primarily cosmetic • Services which are neither performed nor prescribed by a Dentist except for those services of a licensed dental hygien ist which are supervised and billed by a Dentist and which are for: o Scaling and polishing of teeth; or o Fluoride treatments; • Services or appliances which restore or alter occlusion or vertical dimension ; • Restoration of tooth structure damaged by attrition, abrasion or erosion; • Restorations or appliances used for the purpose of periodontal splinting; • implants including, but not limited to any related surgery, placement, restorations, maintenance, and removal • Counseling or instruction about oral hygiene, plaque control, nutrition and tobacco; • Personal supplies or devices including, but not limited to: water picks, toothbrushes, or dental floss; • Decoration, personalization or inscription of any tooth, device, appliance, crown or other dental work; • Missed appointments; • Services: o Covered under any workers’ compensation or occupational disease law; o Covered under any employer liability law; o For which the employer of the person receiving such services is not required to pay; or o Received at a facility maintained by the Employer, labor union, mutual benefit association, or VA hospital; • Services covered under other coverage provided by the Employer; • Temporary or provisional restorations; Type D — Orthodontia N/A You, your spouse and your children, up to age 19, are covered while Dental insurance is in effect All dental procedures performed in connection with orthodontic treatment are payable as Orthodontia Payments are on a repetitive basis 20% of the Orthodontia Lifetime Maximum will be considered at initial placement of the appliance and paid based on the plan benefit’s coinsurance level for Orthodontia as defined in the plan summary Orthodontic benefits end at cancellation of coverage
Metropolitan Life Insurance Company | 200 Park Avenue | New York, NY 10166 L0521014040[exp0622][xNM ] © 2021 MetLife Services and Solutions, LLC DN-ANY-PPO-DU AL PLAN SUMMARY Dental Insurance Bankers Financial Co. • Temporary or provisional appliances; • Prescription drugs; • Services for which the submitted documentation indicates a poor prognosis; • The following when charged by the Dentist on a separate basis: o Claim form completion; o Infection control such as gloves, masks, and sterilization of supplies; or o Local anesthesia, non-intravenous conscious sedation or analgesia such as nitrous oxide. • Dental services arising out of accidental injury to the teeth and supporting structures, except for injuries to the teeth due to chewing or biting of food; • Initial installation of a fixed and permanent Denture to replace one or more natural teeth which were missing before such person was insured for Dental Insurance, except for congenitally missing natural teeth; • Precision attachments, except when the precision attachment is related to implant prosthetics; • Initial installation of a full or removable Denture to replace one or more natural teeth which were missing before such person was insured for Dental Insurance, except for congenitally missing natural teeth; • Addition of teeth to a partial removable Denture to replace one or more natural teeth which were missing before such person was insured for Dental Insurance, except for congenitally missing natural teeth; • Adjustment of a Denture made within 6 months after installation by the same Dentist who installed it; • Fixed and removable appliances for the treatment of harmful habits (Low Plan Only) • Repair or replacement of an orthodontic device; • Repairs of implants • Orthodontic Services (Low Plan Only) • Duplicate prosthetic devices or appliances; • Replacement of a lost or stolen appliance, Cast Restoration, or Denture • Implants supported prosthetics to replace one or more natural teeth which were missing before such person was insured for Dental Insurance, except for congenitally missing natural teeth Limitations Alternate Benefits: Where two or more professionally acceptable dental treatments for a dental condition exist, reimbursement is based on the least costly treatment alternative. If you and your dentist have agreed on a treatment that is more costly than the treatment upon which the plan benefit is based, you will be responsible for any additional payment responsibility. To avoid any misunderstandings, we suggest you discuss treatment options with your dentist before services are rendered, and obtain a pre-treatment estimate of benefits prior to receiving certain high cost services such as crowns, bridges or dentures. You and your dentist will each receive an Explanation of Benefits (EOB) outlining the services provided, your plan’s reimbursement for those services, and your out-of-pocket expense. Procedure charge schedules are subject to change each plan year. You can obtain an updated procedure charge schedule for your area via fax by calling 1-800-942-0854 and using the MetLife Dental Automated Information Service. Actual payments may vary from the pretreatment estimate depending upon annual maximums, plan frequency limits, deductibles and other limits applicable at time of payment. Cancellation/Termination of Benefits: Coverage is provided under a group insurance policy (Policy form GPNP99) issued by Metropolitan Life Insurance Company (MetLife). Coverage terminates when your membership ceases, when your dental contributions cease or upon termination of the group policy by the Policyholder or MetLife. The group policy terminates for non-payment of premium and may terminate if participation requirements are not met or if the Policyholder fails to perform any obligations under the policy. The following services that are in progress while coverage is in effect will be paid after the coverage ends, if the applicable in stallment or the treatment is finished within 31 days after individual termination of coverage: Completion of a prosthetic device, crown or root canal therapy. Like most group benefit programs, benefit programs offered by MetLife and its affiliates contain certain exclusions, exceptions, reductions, limitations, waiting periods and terms for keeping them in force. For complete details of coverage and availability, please refer to the certificate of insurance or contact MetLife.
Metropolitan Life Insurance Company | 200 Park Avenue | New York, NY 10166 L0521014040[exp0622][xNM ] © 2021 MetLife Services and Solutions, LLC DN-ANY-PPO-DU AL PLAN SUMMARY Dental Insurance Bankers Financial Co. Questions & Answers Q. Who is a participating dentist? A. A participating dentist is a general dentist or specialist who has agreed to accept negotiated fees as payment in full for covered services provided to plan members. Negotiated fees typically range from 30% – 45% below the average fees charged in a dentist’s community for the same or substantially similar services.† Q. How do I find a participating dentist? A. There are thousands of general dentists and specialists to choose from nationwide --so you are sure to find one that meets your needs. You can receive a list of these participating dentists online at www.metlife.com/mybenefits or call 1-800-942-0854 to have a list faxed or mailed to you. Q. What services are covered under this plan? A. The certificate of insurance/summary plan description sets forth the covered services under the plan. Please review the enclosed plan benefits to learn more. Q. May I choose a non-participating dentist? A. Yes. You are always free to select the dentist of your choice. However, if you choose a non-participating dentist your out-of-pocket costs may be higher. Q. Can my dentist apply for participation in the network? A. Yes. If your current dentist does not participate in the network and you would like to encourage him/her to apply, ask your dentist to visit www.metdental.com, or call 1-866-PDP-NTWK for an application.†† The website and phone number are for use by dental professionals only. Q. How are claims processed? A. Dentists may submit your claims for you which means you have little or no paperwork. You can track your claims online and even receive email alerts when a claim has been processed. If you need a claim form, visit www.metlife.com/mybenefits or request one by calling 1-800-942-0854. Q. Can I get an estimate of what my out-of-pocket expenses will be before receiving a service? A. Yes. You can ask for a pretreatment estimate. Your general dentist or specialist usually sends MetLife a plan for your care and requests an estimate of benefits. The estimate helps you prepare for the cost of dental services. We recommend that you request a pre-treatment estimate for services in excess of $300. Simply have your dentist submit a request online at www.metdental.com or call 1-877-MET-DDS9. You and your dentist will receive a benefit estimate for most procedures while you are still in the office. Actual payments may vary depending upon plan maximums, deductibles, frequency limits and other conditions at time of payment. Q. Can MetLife help me find a dentist outside of the U.S. if I am traveling? A. Yes. Through international dental travel assistance services* you can obtain a referral to a local dentist by calling +1-312-356-5970 (collect) when outside the U.S. to receive immediate care until you can see your dentist. Coverage will be considered under your out-of-network benefits.** Please remember to hold on to all receipts to submit a dental claim.
Metropolitan Life Insurance Company | 200 Park Avenue | New York, NY 10166 L0521014040[exp0622][xNM ] © 2021 MetLife Services and Solutions, LLC DN-ANY-PPO-DU AL PLAN SUMMARY Dental Insurance Bankers Financial Co. Q. How does MetLife coordinate benefits with other insurance plans? A. Coordination of benefits provisions in dental benefits plans are a set of rules that are followed when a patient is covered by more than one dental benefits plan. These rules determine the order in which the plans will pay benefits. If the MetLife dental benefit plan is primary, MetLife will pay the full amount of benefits that would normally be available under the plan, subject to applicable law. If the MetLife dental benefit plan is secondary, most coordination of benefits provisions require MetLife to determine benefits after benefits have been determined under the primary plan. The amount of benefits payable by MetLife may be reduced due to the benefits paid under the primary plan, subject to applicable law. Q. Do I need an ID card? A. No. You do not need to present an ID card to confirm that you are eligible. You should notify your dentist that you are enrolled in the MetLife Preferred Dentist Program. Your dentist can easily verify information about your coverage through a toll-free automated Computer Voice Response system. †Based on inter nal analysis by M etLife. Neg otiated fees refer to the fees that in-network dentists have ag reed to accept as paym ent in full for covered services, subject to any co-payments, deductibles, cost shar ing and benefits maximums. Neg otiated fees ar e subject to chang e. ††Due to contr actual req uir em ents, MetLife is pr evented fr om soliciting certain providers. *AXA Assistance USA, Inc. provides Dental r eferral services only. AXA Assistance is not affiliated with M etLife, and the services and benefits they pr ovide are separate and apart from the insur ance provided by M etLife. Refer r al ser vices are not available in all locations. **Refer to your dental benefits plan sum mary for your out-of-network dental cover ag e.